Environmental dimensions of antimicrobial resistance
What is the problem?
Understanding and managing the role of the environment in the development and spread of AMR is a vital task towards successfully combatting AMR across the globe. However, the environmental dimensions of AMR have received notably less focus, resources and progress than the human, plant and animal health sectors. Use of antimicrobials in humans, plants and animals all contribute to the environmental load of antimicrobial resistant bacteria, genes, residues and their metabolites; however, the extent to which each are drivers of resistance and negative One Health outcomes in different contexts is not well understood. Without inclusion or consideration of all the drivers and pathways of AMR into the environment, AMR mitigation efforts (e.g. AMR Action Plans) are incomplete and at risk of not achieving the desired goals of protecting and ensuring the efficacy of existing and future antimicrobials.
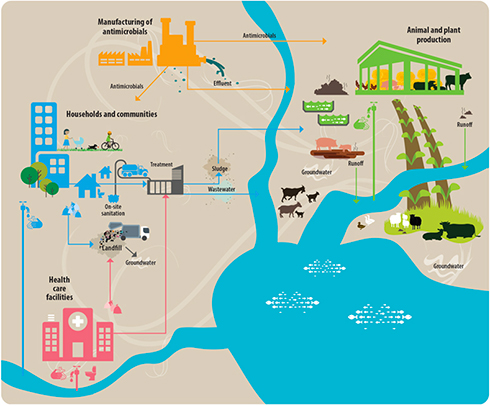
AMR enters the environment through a myriad of pathways. For example, potentially high levels of antimicrobials and, correspondingly, high levels of AMR and antimicrobial resistance genes can be found in waste streams from humans, animals and plants treated with antimicrobials, as well as in the effluent from wastewater treatment plants. The sewage of antimicrobial manufacturing plants entering the environment also might contain more antimicrobial resistant microorganisms and antimicrobial resistance genes than sewage from hospitals or from urban areas. Additionally, soils are contaminated by antimicrobial treatments used for disease control in plant production, and by residues in manures and wastes applied as crop fertilizers. In general, waste streams and wastewater from these activities can act as potential reservoirs, vehicles of transmission, and create environmental hotspots of AMR.
The highly complex, transnational and multisectoral nature of AMR raises important questions about the role the environment plays in the fate and transport of antimicrobials and the development and spread of AMR. A better understanding of how AMR moves from agricultural areas to the environment through soil and water is important for developing guidance towards cost-effective management of AMR and supporting evidence-based, resource-efficient policymaking. The need for strong land and water protection guidelines and policy-frameworks is clear. Effective water supply, sanitation, hygiene and waste management strategies; filling critical research gaps in environmental surveillance and monitoring; and the development and implementation of best management practices to limit AMR in the environment should be a high priority across all sectors as environmental stewardship is a shared multistakeholder responsibility. Currently, the spread of AMR in the environment is generally not controlled by national or international legal regulations.
Challenges and solutions
Most of the existing actions to mitigate AMR reaching the environment from agricultural activities focus on maintaining livestock health and welfare and the responsible and prudent use of antimicrobials by veterinarians and farmers. However, even if those measures are successfully implemented, environmental contamination with antimicrobials will still occur due to their presence in plant production, in excreta and aquaculture systems after prudent application.
While antimicrobial use drives the development of AMR in livestock, aquaculture and plant production, the challenge is that the spread of AMR is fueled by inadequate waste management, pollution, and other non-use factors. Globally, antimicrobials are used in higher quantities in terrestrial and aquatic animal production than in humans; additionally, livestock produce about four times more fecal matter than humans in total. To exacerbate this challenge, as little as 10 to over 80 percent of antimicrobials administered to animals is absorbed or metabolized, with the remainder excreted as active compounds through urine and/or feces in the environment. If not properly managed, wastewater and manure from intensive livestock production and aquaculture systems can be a source of antimicrobial resistant microorganisms, antimicrobial resistance genes, antimicrobial compounds and their metabolites. Runoff waste from slaughterhouses is another potential source of contamination of AMR if not managed properly.
In addition to applying good husbandry practices and prudent use for minimizing AMR in the environment, there are also several options available for properly managing critically important wastewater and manure from livestock and aquaculture production systems to make them safe to be either reused or disposed of. FAO works with a variety of partners and stakeholders to raise awareness and promote their implementation.
Some options can also provide more direct benefits to farmers, such as by generating biogas from waste, or reusing safe and fit-for-purpose water in agricultural activities. In all cases, as a co-benefit, the aim should be to eliminate or drastically reduce the concentration of antimicrobial compounds and resistant organisms in the waste, and options should be selected on a context-specific basis.
For more info please contact:

